Review on ACLS Approach of Pregnancy in Maternal Collapse?
Adel Hamed Elbaih1,2* and Adnan UM Al-Nasser2
1Emergency Medicine Department, Faculty of Medicine, Suez Canal University, Ismailia, Egypt
2Emergency Medicine, College of medicine, Sulaiman AlRajhi University, Clinical Medical Science, Saudi Arabia
*Address for Correspondence: Adel Hamed Elbaih, Faculty of Medicine, Suez Canal University, Ismailia, Egypt, ORCiD: 0000-0002-3347-5163; Tel: + 0020-115-459-9748; E-mail: elbaihzico@yahoo.com; 151110062@srcolleges.org
Submitted: 16 August 2020; Approved: 27 August 2020; Published: 28 August 2020
Citation this article: Elbaih AH, Al-Nasser AU. Review on ACLS Approach of Pregnancy in Maternal Collapse. Int J Case Rep Short Rev. 2020;6(8): 038-00. https://dx.doi.org/10.37871/ijcrsr.id81
Copyright: © 2020 Elbaih AH, et al. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited
Keywords: Maternal collapse; Pregnant women; Emergency physicians; Skill approach
Download Fulltext PDF
Background: Maternal collapse occurs any time during pregnancy, up to 42 days following delivery and is an acute event involving cardiorespiratory systems and/or brain, resulting in impaired consciousness or death. Therefore, we aim to look into the common pitfalls that both medical students and new physicians face in the recognition, diagnosis, and management of these conditions.
Targeted Population: Maternal collapse patients who are requiring urgent management in the ED, with Emergency Physicians for teaching approach protocol.
Aim of the study: Appropriate for identification of women at risk and review of maternal collapse with neonatal outcomes by training protocol to Emergency Physicians. Based on patients’ causes of maternal collapse pregnant women.
Methods: Collection of all possible available data about the Pregnancy in Maternal Collapse in the Emergency department. By many research questions to achieve these aims so a midline literature search was performed with the keywords “critical care”, “emergency medicine”, “principals of ACLS therapy in Pregnancy “, “ACLS and Maternal Collapse”. Literature search included an overview of recent definition, causes and recent therapeutic strategies.
Results: All studies introduced that the initial diagnosis of Pregnancy in Maternal Collapse and their therapy is a serious condition that face patients of the emergency and critical care departments.
Conclusion: Emergency obstetric care to address the major causes of maternal death, Postnatal care which is the six weeks following delivery and Public health approach to decrease with addressing maternal mortality.
Introduction & Definition
Post-partum collapse (Maternal collapse) is fortunately a rare condition worldwide. However, when it occurs, it may be life threatening. The outcome, primarily for the mother but also for the fetus, depends on prompt and effective resuscitation. As a health care provider, the primary goal is immediate and effective resuscitation of the woman to ensure adequate oxygenation and effective cardiac output. Once resuscitation has commenced, every effort must be made to elucidate the cause and instigate effective treatment [1].
Maternal collapse occurs any time during pregnancy, up to 42 days following delivery and is an acute event involving cardiorespiratory systems and/or brain, resulting in impaired consciousness or death [2].
In other words, maternal collapse is any event that affects the cardiorespiratory or brain that results in reduced or absent consciousness. A collapse may be as simple as a vasovagal episode or it may be a cardiac event with unfavorable outcomes. It may occur at any stage in pregnancy until six weeks post-partum and may, despite all efforts, result in the death of the mother and baby. Causes of maternal collapse, with a mnemonic, can be seen in Table 1 & 4 [3].
Postpartum collapse is a rare but very dangerous condition. Outcome for the mother and fetus depends on prompt and effective resuscitation. The true rate of maternal collapse lies somewhere between 0.14 and 6/1000 (14 and 600/100 000) births. The main challenge lies in the diagnosis of the disease, different treatment protocols, multiple risk factors, etiology, and outcomes. In this connection, the question arises regarding an integrated approach to the study of this condition and the development of recommendations for the management of patients of this kind, which served as the purpose of this manuscript [4].
The incidence of the problem
When it comes to the incidence of this condition, it is difficult to determine an accurate rate of maternal collapse. But generally speaking; maternal deaths are generally quantified as a Maternal Mortality Ratio (MMR), expressed as the number of maternal deaths per 100,000 women giving birth. It includes deaths that occur due to complications of the pregnancy (direct deaths), and those resulting from worsening of other disease processes due to the pregnancy (indirect deaths). Deaths that occur from causes completely unrelated to pregnancy or birth are termed incidental deaths, and are not included in calculation of the MMR [4].
Severe maternal morbidity data was collected Scotland-wide for 5 years and published in 2007.3 A woman was defined as having had a severe maternal morbidity event if there was a risk of maternal death without timely intervention. The data showed a severe maternal morbidity rate of 6/1000 (600/100 000) maternities, but not all cases of severe maternal morbidity involved maternal collapse (although all cases of collapse were included in the figures). A recent publication from Dublin showed a severe maternal morbidity rate of 3.2/1000 (320/100 000) births. In the last triennium in the UK the maternal mortality rate was 14/100 000 births,1 but again not all maternal deaths are preceded by maternal collapse. Thus, the true rate of maternal collapse lies somewhere between 0.14 and 6/1000 (14 and 600/100 000) births [5].
Anyway, as I have previously pointed, maternal collapse is considered a rare condition, but maternal death even rarer. Not all maternal deaths are preceded by an identifiable collapse, and not all maternal collapses result in death.
Why this is a problem? (Scope of the problem and Rational to this research topic)
This medical condition is considered a challenge when it encounters the health care-team and there are different protocols for its management even though it’s a rare one, this is because it includes a wide-range of risk factors, etiologies and outcomes taking these significant points into consideration.
This descriptive study aims to highlight
♦ The identification of women at increased risk of maternal collapse comparing to those who are not.
♦ To briefly illustrate the different causes of maternal collapse.
♦ Also, to delineate the initial and continuing management of this condition as the recent protocols advice, and to review maternal and neonatal outcomes.
♦ Furthermore, it’s necessary to clarify another important query regarding if there are possible ways to prevent or reduce the maternal collapse or not?
Methodology
This section includes Collection of all possible available data about the Pregnancy in Maternal Collapse in the Emergency department. By many research questions to achieve these aims so a midline literature search was performed with the keywords “critical care”, “emergency medicine”, “principals of ACLS therapy in Pregnancy “, “ACLS and Maternal Collapse”. All studies introduced that the initial diagnosis of Pregnancy in Maternal Collapse and their therapy is a serious condition that face patients of the emergency and critical care departments. Literature search included an overview of recent definition, causes and recent therapeutic strategies.
So the main aims and outcome of the study: initial assessment and evaluate the suspected maternal collapse patient’s presentation to recognize potentially life-threatening conditions and to convey life-saving treatment so the key note here is that initial diagnosis in suspected cases with treatment.
While searching for this study, the RCOG - (Royal College of Obstetricians and Gynecologists), Medline website and PubMed were searched for relevant the search was restricted to articles published between 1960 and 2011.
The databases were searched using the relevant MeSH terms, including all subheadings, and this was combined with a keyword search. Search words included “Maternal Collapse” ‘amniotic fluid embolism’, ‘cardiac arrest and pregnancy’, ‘DVT and pregnancy’, ‘hypovolemia and pregnancy’, ‘hypoxia and pregnancy’, ‘massive haemorrhage’, ‘maternal collapse’ and ‘resuscitation and pregnancy’ ’Prevention’. The search was also limited to humans and the English language. The National Library for Health and the National Guidelines Clearing House were also searched for relevant guidelines and reviews.
What are the risk factors of maternal collapse?
Cardiovascular diseases.
Psychosocial causes; this includes suicide, drug and alcohol use, and domestic violence.
Maternal age 35 and older.
Obesity.
Lower socioeconomic status.
Pre-existing mental health issues, substance use and domestic violence, all of which may be exacerbated by pregnancy and the puerperium.
Medical co-morbidities, particularly asthma, autoimmune diseases, inflammatory and atopic disorders, hematological disorders, essential hypertension, infections and musculoskeletal disorders.
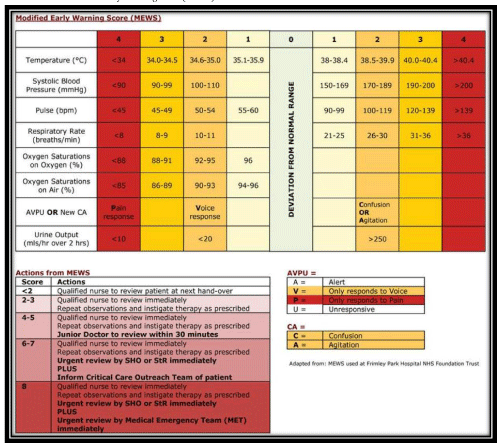
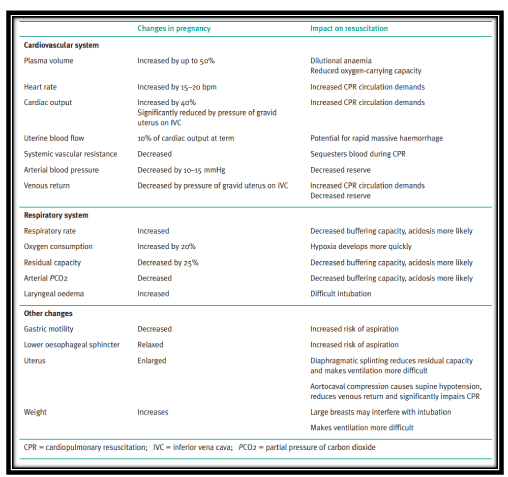
Moreover, one of the important developments in improving identification of a pregnant or postnatal patient at risk of collapse during hospital admission has been the development of maternity-specific Early Warning Charts. These charts for regular observations consider the altered physiology of pregnancy (Table 3), and provide clear guidelines for when observations fall outside the realm of expected or acceptable, thereby triggering an alert to the responsible obstetrician. These charts make recognition of a deteriorating maternity patient much easier, allowing timely medical intervention. All units responsible for the care of pregnant and postnatal patients should have such charts available and in use. (Table 2) [6].
What are the different causes of maternal collapse?
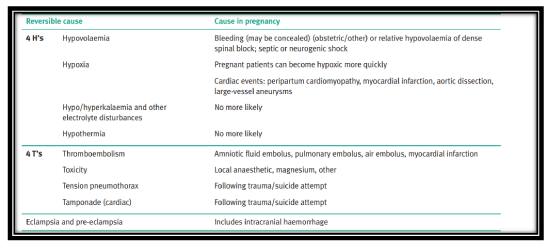
There are many causes of collapse, and these may be pregnancy-related or result from conditions not related to pregnancy and possibly existing before pregnancy. Systematic consideration of the causes of collapse can enable skilled rescuers to identify the cause of collapse in the hospital setting and, where the cause is reversible, survival can be improved.19 The common reversible causes of collapse in any woman can be remembered using the well-known ‘aide memoire’ employed by the Resuscitation Council (UK) of the 4 T’s and the 4 H’s.19 In the pregnant woman, eclampsia and intracranial hemorrhage should be added to this list, and obstetric-specific causes are clearly more likely and must also be considered systematically. (Table 4) [7].
Hemorrhage: According to the CEMACH (Confidential Enquiry into Maternal and Child Health). This is the most common cause of maternal collapse, and was responsible for 17 maternal deaths in the last triennium. Major obstetric hemorrhage has an estimated incidence of 3.7/1000 maternities. Causes of major obstetric haemorrhage include postpartum haemorrhage, major antepartum haemorrhage from placenta praevia/ accreta, placental abruption, uterine rupture and ectopic pregnancy. In most cases of massive haemorrhage leading to collapse, the cause is obvious, but concealed haemorrhage should not be forgotten, including following caesarean section and ruptured ectopic pregnancy. Other rarer causes of concealed haemorrhage include splenic artery rupture21 and hepatic rupture [8].
Thromboembolism: In the last CEMACH report, there were 41 deaths from thromboembolism (33 pulmonary embolism and eight cerebral vein thrombosis), making it the most common cause of direct maternal death. Appropriate use of thromboprophylaxis has improved maternal morbidity and mortality, but improvements in clinical risk assessment and prophylaxis are still required [8].
Amniotic fluid embolism: The estimated frequency of Amniotic Fluid Embolism (AFE) lies somewhere between 1.25/100 000 and 12.5/100 000 maternities, with the most recent UK data giving an incidence of 2/100 000 maternities. Survival rates seem to have improved significantly over time. The perinatal mortality. Rate in cases of AFE is 135/1000 total births. AFE presents as collapse during labor or delivery or within 30 minutes of delivery in the form of acute hypotension, respiratory distress and acute hypoxia. Seizures and cardiac arrest may occur [9].
Cardiac disease: Cardiac disease was the most common overall cause of maternal death in the CEMACH report,1 being responsible for 48 maternal deaths. The majority of deaths secondary to cardiac causes occur in women with no previous history. The main cardiac causes of death are myocardial infarction, aortic dissection and cardiomyopathy.1 The incidence of primary cardiac arrest in pregnancy is much rarer at around 1/30 000 maternities, and most cardiac events have preceding signs and symptoms. Aortic root dissection can present in otherwise healthy women, and signs and symptoms such as central chest or interscapular pain, a wide pulse pressure, mainly secondary to systolic hypertension, and a new cardiac murmur must prompt referral to a cardiologist and appropriate imaging. The incidence of congenital and rheumatic heart disease in pregnancy is increasing secondary to increased survival rates owing to improved management of congenital heart disease and increased immigration [10].
These cases should be managed by an appropriately skilled and experienced multidisciplinary team, usually in regional centers. Other cardiac causes include dissection of the coronary artery, acute left ventricular failure, infective endocarditis and pulmonary edema.
Sepsis: Sepsis has been recognized for centuries as a significant cause of maternal morbidity and mortality, and substandard care continues to feature in the cases that result in death. Bacteremia, which can be present in the absence of pyrexia or a raised white cell count, can progress rapidly to severe sepsis and septic shock leading to collapse; the most common organisms implicated in obstetrics are the streptococcal groups A, B and D, pneumococcus and Escherichia coli [11].
Drug toxicity/overdose: Drug toxicity/overdose should be considered in all cases of collapse, and illicit drug overdose should be remembered as a potential cause of collapse outside of hospital. In terms of therapeutic drug toxicity, the common sources in obstetric practice are magnesium sulphate in the presence of renal impairment and local anesthetic agents injected intravenously by accident.
Toxic effects associated with local anesthetics usually result from excessively high plasma concentrations. Effects initially include a feeling of inebriation and lightheadedness followed by sedation, circumoral paranesthesia and twitching; convulsions can occur in severe toxicity. On intravenous injection, convulsions and cardiovascular collapse may occur very rapidly. Local anesthetic toxicity resulting from systemic absorption of the local anesthetic may occur sometime after the initial injection. Signs of severe toxicity include sudden loss of consciousness, with or without tonic–colonic convulsions, and cardiovascular collapse: sinus bradycardia, conduction blocks, asystole and ventricular tachyarrhythmias can all occur [12].
Eclampsia: Eclampsia as the cause of maternal collapse is usually obvious in the inpatient setting, as often the diagnosis of pre-eclampsia has already been made and the seizure witnessed. Epilepsy should always be considered in cases of maternal collapse associated with seizure activity
Intracranial haemorrhage: Intracranial haemorrhage is a significant complication of uncontrolled, particularly systolic, hypertension, but can also result from ruptured aneurysms and arteriovenous malformations. The initial presentation may be maternal collapse, but often severe headache precedes this [13].
Anaphylaxis: Anaphylaxis is a severe, life-threatening generalized or systemic hypersensitivity reaction35 resulting in respiratory, cutaneous and circulatory changes and, possibly gastrointestinal disturbance and collapse. There is significant intravascular volume redistribution, which can lead to decreased cardiac output. Acute ventricular failure and myocardial ischemia may occur. Upper airway occlusion secondary to angioedema, bronchospasm and mucous plugging of smaller airways all contribute to significant hypoxia and difficulties with ventilation. Common triggers are a variety of drugs, latex, animal allergens and foods. The incidence is between 3 and 10/1000, with a mortality rate of around 1%.36 Anaphylaxis is likely when all of the following three criteria are met:
➣ Sudden onset and rapid progression of symptoms.
➣ Life-threatening airway and/or breathing and/or circulation problems.
➣ Skin and/or mucosal changes (flushing, urticarial, angioedema) [13].
Other causes: Other causes of maternal collapse include hypoglycemia and other metabolic/electrolyte disturbances, other causes of hypoxia such as airway obstruction secondary to aspiration/foreign body, air embolism, tension pneumothorax, cardiac tamponade secondary to trauma and hypothermia. There will be other very unusual and rare causes of maternal collapse, but detailed discussion of all causes is beyond the scope of this article.
What is the best approach for management of maternal collapse?
To achieve the optimal initial management of maternal collapse during maternal resuscitation, your methods should follow the Resuscitation Council (UK) guidelines using the standard A, B, C approach, with some modification, as I will demonstrate:
It worth to mention that, in the UK, resuscitation is conducted according to the UK Resuscitation Council Guidelines: Basic Life Support (BLS), Adult Advanced Life Support (ALS) and Automated External Defibrillation (AED) algorithms and recommendations. (Appendix1 & 2) These guidelines were updated in 2010 by international experts under the auspices of the International Liaison Committee on Resuscitation and are used in the resuscitation of the pregnant woman [14].
First Step: Immediate action: Summon help!
✓ Fast Bleep Obstetric on call team consisting of junior grade doctor.
✓ Middle grade and Maternity Anesthetist.
✓ Inform Coordinator on Labor Ward if on other relevant area.
✓ Inform consultant Obstetrician on call.
✓ Bleep neonatal team if beyond 22-week gestation.
✓ Crash trolley with AED must be made available immediately to facilitate resuscitation.
Assess the patient!
✓ A - Airway - remove false teeth, blood, vomit etc. using fingers or suction apparatus.
✓ B - Breathing -Ambu Bag and mask or Guedel airway.
✓ C - Circulation - in the absence of breathing commence cardiac compressions as per the Resuscitation Council UK Guidelines. Whilst carrying out CPR, gain IV access with large bore cannula14/16 G(Grey/Orange), bloods for investigations including random blood glucose and commence fluid resuscitations.
✓ Defibrillation/Drugs-Pregnant women should be treated no differently than any other adult patient when considering drugs or energy for defibrillation.
Next, Tilt the patient!
✓ A left lateral tilt of 15 degree on a firm surface will relieve aortocaval compression in the majority of pregnant women and allows effective chest compressions to be performed.
✓ Alternatively, gravid uterus can be manually displaced to the maternal left to relieve aortocaval compression and facilitate CPR.
✓ If patient has suffered cardiac or respiratory arrest call the arrest team Commence CPR.
✓ Generally, what recent protocols advice is to Commence Cardio Pulmonary Resuscitation (CPR) immediately with manually tilting the uterus (for women > 20 weeks gestation).
✓ Commence cardiac compressions at the rate of 100-120 beats per minute and give 2 breaths via mouth to mouth or Ambu bag and mask ventilation for every 30 compressions.
✓ If no cardiac output by 4 minutes a perimortem caesarean section must be carried out regardless of the fetal condition and must be completed by 5min.
✓ Cesarean section should be performed where resuscitation is taking place and should not be delayed by moving the patient.
✓ A sterile scalpel blade and cord clamps must be available on the crash trolley.
✓ CPR should be continued throughout the surgery.
✓ Adhesive pads are preferred to paddles for defibrillation and pads must be placed on lateral to left breast and on anterior surface of right clavicular area. CPR must be continued until a shock is delivered.
✓ Ensure to remove the oxygen and uterine monitors on patient and ensure staff are well away from patient before administering shock, if shockable rhythm.
✓ Commence CPR immediately after delivering shock.
✓ If non shockable rhythm, continue CPR.
✓ Give adrenaline every 3-5 min. Assess patient continuously for any reversible causes.
✓ Resuscitation efforts should be continued until a decision is taken by the consultant obstetrician, and consultant anesthetist in consensus with the cardiac arrest team.
✓ Transfer to critical care team when successfully resuscitated [14].
Secondary action: These will include:
✓ Gain venous access, take blood for FBC, group and save, clotting screen, cardiac enzymes, U&E, LFT& serum glucose. Cross match 6 units of blood.
✓ Check oxygen saturation using a pulse oximetry.
How to deal with different causes when you suspect them?
Pulmonary embolus: A prodromal of anxiety, chest pain tachycardia and shortness of breath may have been present. A DVT may have been diagnosed. Oxygen saturation may be poor. Cardiac arrest is characterized by electromechanical dissociation.
• Management
✓ Maintain oxygenation.
✓ Prolonged cardio-pulmonary resuscitation may break up the thrombus.
✓ Maintain BP with crystalloid infusion.
✓ Anti-coagulate with an IV bolus of 10 000 units of heparin with senior input.
✓ Consider thrombolytic agents with senior input and discuss this with them [15].
Eclampsia: Pre-eclampsia may have been present or absent. The patient will be fitting it’s criteria.
• Management
Follow Management of Eclampsia Protocol.
Amniotic fluid embolus: Acute shortness of breath, cough with frothy pink sputum and cyanosis, followed by apnea, cyanosis and shock are typical of amniotic fluid embolus. Seizures may occur, DIC and renal failure may follow.
• Management
✓ Maintain airway, will usually require intubation and ventilation.
✓ Maintain BP using Normal Saline.
✓ Inform hematologists of diagnosis.
✓ Maintain Hb using blood transfusion.
✓ Correct thrombocytopenia with platelet infusion.
✓ Replace clotting factors with FFP [16].
Myocardial infarction: The pain is typically retrosternal and crushing, nausea and shortness of breath are common.
• Management
✓ Control pain with i.v. diamorphine and LVF with i.v. Frusemide.
✓ Correct arrhythmias as determined by ECG strip.
✓ Administer 100% oxygen. If in complete heart block maintain the ventricular rate with i.v. atropine until able to pace [17].
Drug toxicity: i. Opioids: Administered by any route may cause respiratory depression. Increasing sedation, decreasing respiratory rate and finally falling oxygen saturation predate respiratory arrest.
• Management:
✓ Discontinue any opioid therapy, administer oxygen, basic life support, administer intravenous naloxone (initially 0.4mg, repeated and infusion if necessary).
ii. Local anesthetic accidental intravenous injection: Characterized by prodrome of perioral tingling, light-headiness, tinnitus. Followed by seizures and cardiovascular collapse.
• Management
✓ Stop injection, administer oxygen, basic life support, seizure control with attention to securing airway Give IV bolus injection of Intralipid 20% 1.5 ml/kg over 1 minute (100 ml for a 70 kg woman) followed by an intravenous infusion of Intralipid 20% at 0.25 ml/kg/min (400 ml over 20 minutes for a 70 kg woman).
✓ The bolus injection can be repeated twice at 5-minute intervals if an adequate circulation has not been restored (a further two boluses of 100 ml at 5-minute intervals for a 70 kg woman).
✓ After another 5 minutes, the infusion rate should be increased to 0.5 ml/kg/ min.
✓ If adequate circulation has not been restored. CPR should be continued throughout this process until an adequate circulation has been restored, and this may take over an hour [18].
Sepsis: Must be managed as per management of maternal sepsis guidelines.
Anaphylaxis: The definitive treatment for anaphylaxis is 500 micrograms (0.5 ml) of 1:1000 adrenaline intramuscularly. Adjuvant therapy consists of chlorpheniramine 10 mg and hydrocortisone 200 mg. Both are given intramuscularly or by slow intravenous injection.
Hypoglycaemia: Blood glucose levels less than 4.0mmol/L; Generally, any blood glucose less than 4.0mmol/L should be treated.
• Management of hypoglycemia in unconscious women
✓ If the patient has an insulin infusion in situ, stop immediately.
✓ If IV access available, give 75-100ml of 20% glucose over 15 minutes, (e.g. 300-400ml/hr.)).
✓ Repeat capillary blood glucose measurement 10 minutes later. If it is still less than 4.0mmol/L, repeat.
✓ If IV access is difficult and is going to take longer than 15 minutes, glucagon 1mg IM can be given as an alternative. It may take up to 15 minutes to be effective [19].
What are the outcomes for mother and baby? : Owing to the lack of robust population data, it is not possible to be accurate regarding outcomes. It is widely accepted that there is significant selection bias in publications relating to the topic. The Confidential Enquiries into Maternal Death have given robust data when resuscitation was not successful, and the Scottish Maternal Morbidity data3 and the Dublin study4 report maternal survival figures for severe maternal morbidity, but not for collapse per se. These data do give ‘near miss’ to death ratios of 56:13 and 79:1.4 For some conditions such as AFE, the maternal survival figures are more robust, but accurate data collection is required for maternal collapse as a whole [15].
Is there a possible way to prevent maternal collapse?
In fact, almost all of the causes that we have discussed are either preventable or have highly effective interventions. Another factor that contributes to the maternal mortality rate that have opportunities for prevention are access to prenatal care for women who are pregnant. Women who do not receive prenatal care are between three and four times more likely to die from complications resulting from pregnancy or delivery than those who receive prenatal care. For women in the United States, 25% do not receive the recommended number of prenatal visits, and this number increases for women among specific demographic populations: 32% for African American women and 41% for American Indian and Alaska Native women.
Four elements are essential to maternal death prevention, according to UNFPA (United Nations Population Fund)
✓ First, prenatal care. It is recommended that expectant mothers receive at least four antenatal visits to check and monitor the health of mother and fetus.
✓ Second, skilled birth attendance with emergency backup such as doctors, nurses and midwives who have the skills to manage normal deliveries and recognize the onset of complications.
✓ Third, emergency obstetric care to address the major causes of maternal death which are hemorrhage, sepsis, unsafe abortion, hypertensive disorders and obstructed labor.
✓ Lastly, postnatal care which is the six weeks following delivery. During this time, bleeding, sepsis and hypertensive disorders can occur, and newborns are extremely vulnerable in the immediate aftermath of birth. Therefore, follow-up visits by a health worker to assess the health of both mother and child in the postnatal period is strongly recommended.
✓ Additionally, Maternal Death Surveillance and Response is another strategy that has been used to prevent maternal death. This is one of the interventions proposed to reduce maternal mortality where maternal deaths are continuously reviewed to learn the causes and factors that led to the death. The information from the reviews is used to make recommendations for action to prevent future similar deaths.
✓ Furthermore, Medical technologies the decline in maternal deaths has been due largely to improved aseptic techniques, better fluid management and quicker access to blood transfusions, and better prenatal care.
✓ Not only this but also, some maternal deaths can be prevented through medication use. Injectable oxytocin can be used to prevent death due to postpartum bleeding [8]. Additionally, postpartum infections can be treated using antibiotics. In fact, the use of broad-spectrum antibiotics both for the prevention and treatment of maternal infection is common in low-income countries [5,4]. Maternal death due to eclampsia can also be prevented through the use of medications such as magnesium sulfate.
✓ Finally, A public health approach to addressing maternal mortality includes gathering information on the scope of the problem, identifying key causes, and implementing interventions, both prior to pregnancy and during pregnancy, to combat those causes and to reduce their risks [15,20].
Conclusion & Recommendation
✓ Maternal collapse is an acute event involving the cardiorespiratory system and/or brain, causing reduced or absent conscious level at any point during pregnancy and up to 6 weeks postpartum.
✓ As collapse is not a reported event, the true incidence is difficult to estimate but it could be as high as 6:1000 births.
✓ The most common causes of collapse are vasovagal and epilepsy. While, the most common cause of death is the bleeding.
✓ Many cases are unpredictable, but some can be preceded by general deterioration as documented on observation charts.
✓ Physiological changes in pregnancy means that standard early warning scores cannot apply to pregnancy, and even those modified for pregnancy have failed to show changes in mortality and morbidity.
✓ However, the use of modified EWS is considered good practice.
✓ All clinical staff should have adequate & up to date resuscitation skills.
✓ There must be more efforts provided to apply the methods of prevention of maternal collapse, as the recent studies show, that the prevention of maternal collapse is possible to some extent; these involves:
✓ Prenatal care.
✓ Skilled birth attendance with emergency backup such as doctors, nurses and midwives who have the skills and experience to deal with this condition
✓ Emergency obstetric care to address the major causes of maternal death.
✓ Postnatal care which is the six weeks following delivery.
✓ Public health approach to addressing maternal mortality.
- Elbaih AH, Taha M, Elsakaya MS, Elshemally AA, Alshorbagy ME. Assessment of cardiopulmonary resuscitation knowledge and experiences between emergency department nurses hospital pre and post basic life support training course, Egypt. Annals of Medical Research. 2019; 26: 2320-2327. https://bit.ly/34C7MZS
- Maternal collapse in pregnancy and the puerperium. Royal College of Obstetricians and Gynaecologists (RCOG). 2011. https://bit.ly/2Emilpp
- Development of RCOG Green-top Guidelines: Producing a Clinical Practice Guideline. Royal College of Obstetricians and Gynaecologists (RCOG). 2006. https://bit.ly/34C8R3S
- Taha M, Elbaih A. Pathophysiology and management of different types of shock. NMJ. 2017; 6: 14-39.
- Confidential Enquiry into Maternal and Child Health. Saving Mothers’ Lives: Reviewing maternal deaths to make motherhood safer - 2003-2005. The seventh report of the confidential enquiries into maternal deaths in the United Kingdom. London: CEMACH; 2007.
- Knight M, Kurinczuk JJ, Tufnell D, Brocklehurst P. The UK Obstetric surveillance system for rare disorders of pregnancy. BJOG. 2005: 112: 263-265. DOI: 10.1111/j.1471-0528.2005.00609.x
- Elbaih AH, Elzeky EA, Elshaboury I, Oraby M. A comparative study of risk stratifications scores for acute heart failure patients in the emergency department, Egypt. Int J Surg Med. 2017; 3: 140-149. DOI: 10.5455/ijsm.acute-heart-failure
- Scottish Confidential Audit of Severe Maternal Morbidity. 5th Annual Report. Edinburgh: NHS Quality Improvement Scotland. NHS Quality Improvement Scotland. 2007. https://bit.ly/2EuPy1O
- Elbaih AH, Housseini AM, Khalifa ME. Accuracy and outcome of Rapid Ultrasound in Shock and Hypotension (RUSH) in Egyptian polytrauma patients. Chinese J Traumatology. 2018; 21: 156-162. DOI: 10.1016/j.cjtee.2017.06.009 a
- Mhyre JM, Tsen LC, Einav S, Kuklina EV, Leffert LR, Bateman BT. Cardiac arrest during hospitalization for delivery in the United States, 1998-2011. Anesthesiology. 2014; 120: 810-818. DOI: 10.1097/ ALN.0000000000000159
- Royal College of Obstetricians and Gynaecologists (RCOG), Royal College of Midwives (RCM) and National patient safety agency (NPSA). Safe practice in intrapartum care project. Care bundles. 2010. https://bit.ly/3jmAHp8
- Poon LC, Yang H, Dumont S, Lee JCS, Copel JA, Danneels L, et al. ISUOG Interim Guidance on coronavirus disease 2019 (COVID‐19) during pregnancy and puerperium: Information for healthcare professionals - an update, Ultrasound in Obstetrics & Gynecology. 2020; 55: 848-862. https://bit.ly/3gvc2Nf
- Elbaih AH, Basyouni FH.Teaching Approach of Primary Survey in Trauma Patients. SunText Rev Surg. 2020; 1: 1-7.
- Mortality rates at the dublin maternity hospital 1784-1849.
- "Trends in maternal mortality: 1990 to 2015". World Health Organization. 2015: 16. https://bit.ly/34F3q4q
- Elbaih AH, MohammedElsayed Z, MahmoudAhmed R, AhmedAbd-elwahed S. Sepsis Patient Evaluation Emergency Department (SPEED) score & Mortality in Emergency Department Sepsis (MEDS) score in predicting 28-day mortality of emergency sepsis patients, Chinese Journal of Traumatology. 2019; 22: 316-322. https://bit.ly/2QsvkIe
- Berg C, Danel I, Atrash H, Zane S, Bartlett L. Strategies to reduce pregnancy-related deaths: From identification and review to action. Atlanta: Centers for Disease Control and Prevention. 2001.
- Knaus WA, Zimmerman JE, Wagner DP, Draper EA, Lawrence DE. APACHE - acute physiology and chronic health evaluation: A physiologically based classification system. Crit Care Med. 1981; 9: 591-597. DOI: 10.1097/00003246-198108000-00008
- Whitty JE. Maternal cardiac arrest in pregnancy. Clin Obstet Gynecol. 2002; 45: 377-392. DOI: 10.1097/00003081-200206000-00009
- Elbaih AH. Different types of triage. Arşiv kaynak tarama dergisi. Archives Medical Review Journal. 2017; 26: 441-467.


Sign up for Article Alerts