Sleep Quality and Depression among Undergraduate Medical and Allied Medical Sciences Students: A Cross-Sectional Study At Umm Al-Qura University (Uqu)
Muhammad I Siddiqui*, Asim M Zowgar, Ammar A Almaghrabi and Wafaa M Almalki
Department of Community Medicine, College of Medicine, Umm Al-Qura University, Makkah, Saudi Arabia
*Address for Correspondence: Muhammad Irfanullah Siddiqui, Department of Community Medicine, College of Medicine, Umm Al-Qura University, Makkah, Saudi Arabia,Tel: + 009-665-990-607-13; E-mail: irfan7255@yahoo.com; irfan7255@gmail.com
Submitted: 04 July 2020; Approved: 20 July 2020; Published: 22 July 2020
Citation this article: Siddiqui MI, Zowgar AM, Almaghrabi AA, Almalki WM. Sleep Quality and Depression among Undergraduate Medical and Allied Medical Sciences Students: A Cross-Sectional Study At Umm Al-Qura University (Uqu). Int J Sleep Disord. 2020;3(1): 007-016.
Copyright: © 2020 Siddiqui MI, et al. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited
Keywords: Sleep quality; Depression; Medical students; Pittsburgh Sleep Quality Index; Patient Health Questionnaire-9; Makkah
Download Fulltext PDF
Background: Medical field is considered as high load and stressful field which begins from the day, student is enrolled in medical college, which may negatively affect his life and put him at risk for psychological problems. The purpose of this study was to determine prevalence of sleep quality and depression among medical and allied medical sciences students and find the relationship between sleep quality and depression with different variables
Methods and Materials: A cross-sectional study was conducted among students in medical, dental and pharmacy colleges. Students were randomly selected to fill Pittsburgh Sleep Quality Index (PSQI) for sleep quality and Patient Health Questionnaire (PHQ-9) for depression plus many questions, related to study object. The sampling technique used was multistage random and sample size was 681.
Result: 681 students enrolled in this study. In general, 71.4% had poor sleep quality with mean score 7.47 ± 3.19 and 81.4% had depression with mean score 9.54 ± 5.32 and 19.5% had suicidal ideation. Male had less depression and better sleep quality than female. Highest level of poor sleep quality was in pharmacy students, with 75.3% followed by dentistry 74.4% and lowest in medical students 69.2% and highest level of depression, 88.9%, was in dental students followed by medical students 80.7% and pharmacy students 79%. No significant association was observed between collage, academic year, marital status, economic status, health problem, smoking, regular attendance, GPA, cold or hot drink with sleep quality or depression. About 10.3% of students used sleep medication. Sleep quality, depression and suicidal ideation were significantly associated with each other’s (p < 0.000)
Limitations: We wanted to include all departments of Allied medical sciences but could not get permission from the applied medical sciences, hence the result represent the depression rate in medical, pharmacy and dental students only.
Conclusion: The studied population had significantly high depression rate and poor sleep quality as compare to general population. The two scales of depression and sleep quality were significantly associated. Pharmacy students had highest percentage of poor sleep quality and dental students had highest level of depression. A detailed study should be conducted to find out the factors responsible for higher rates in the two faculties, in order to suggest the appropriate strategy to minimize the depression and poor sleep quality rate.
Introduction
A good sleep is essential for the repair and normal maintenance of good health. Good sleep does not mean sleeping for a long time neither short time as both associated with increased risk for cardiovascular disease, hypertension, obesity and diabetes [1]. Daniel J. Buysse defined Sleep health as “multidimensional pattern of sleep-wakefulness, adapted to individual, social, and environmental demands, that promotes physical and mental well-being” [2]. These dimensions include 5 concepts: sleep duration, sleep continuity or efficiency, timing, alertness/sleepiness and satisfaction/quality. Sleeping behaviors are affected by genes as it is heritable from parents [3]. Cognitive and motor functions are affected in case of moderate sleep deprivation and its effect similar to alcohol consumption at its highest legal limit or above it [4]. Sleep behaviors and psychiatric disorders (including depression) believes to be causative of each other that’s mean sleep problems lead to depression and depression lead to problems in sleep [5]. One of the common questionnaires to assess sleep quality is Pittsburg Sleep Quality Index (PSQI) and for screening depression, Patient Health Questionnaire (PHQ-9) [6,7]. The objectives of this research are 1) To determine prevalence of sleep quality and depression among medical and allied medical sciences students and 2) To find the relationship between sleep quality and depression with different variables.
Methods
Setting: This study was conducted at Umm Al-Qura University (UQU) in Makkah, Saudi Arabia. This university has about 100,000+ students in different campus of the university. The university has 2190 students in medical and allied medical sciences (dentistry and pharmacy). There are four faculties involved in teaching medicine including medical college, dental college, Pharmacy College and applied Medicine College. We were not given consent by the administration of applied medicine college administration and we had to limit our study to only three institutions.
Study design: observational cross-sectional study
Tools for measurements: Pittsburgh Sleep Quality Index (PSQI) (sensitivity 89.6% and specificity 86.5%) and it contains 18 questions composed of 7 components: subjective sleep quality, sleep latency, sleep duration, sleep efficiency, sleep disturbance, use of sleep medication and day time dysfunction to assess sleep quality during last month. Each component has score ranged from 0 to 3 with global score out of 21. Score 5 or less represent good sleep quality whereas score above 5 represent poor sleep quality [6].
Patient Health Questionnaire (PHQ-9) (sensitivity 80% and specificity 92%) to screen for depression and suicidal ideation and it contains 9 items with global score out of 27. Score between 0-4 indicate none or minimal depression (we considered this group as none or no depression), 5-9 mild depression, 10-14 moderate depression, 15-19 moderately severe and 20-27 severe [7].
Many questions were added that related to marital and socioeconomic status, health problems, regular attendance, GPA, smoking, drinking tea or coffee (hot drink) and energy or soft drinks (cold drink) consumption in order to find the association of depression and sleep quality with the above-mentioned factors
Study population: The Population of study is all undergraduate medical, dental, pharmacy students in Umm Al-Qura University from first year to final year. Total study population is 2190 students (1090 male and 1100 female). Medical, pharmacy and dental students represent about 63%, 23.8% and 13.2% respectively. First and second year at medicine and dentistry are preclinical year while third, fourth and fifth are clinical years.
Sample size: Epi-info software of Centre for Disease Control (CDC) was used to calculate sample size. The power of study set at 90, while absolute precision was kept at 5% and the prevalence from a previous study of 36.6% was taken to calculate the final sample size [8]. We found a sample size of 681 with 99% confidence interval. A list of all students registered was obtained from the academic office of each college and a random sample were selected for each year from each college.
The sample size was distributed between specialties according to their proportion of study population. The population was further stratified by gendering, number of fifth year male medical students is 128 that represent 5.84% of study population hence 5.84% of sample size was from fifth year male medical students that is about 40 students and in this way the sample size was distributed. We used Chi Square test of significance for Table 1 and 5 as the data was categorical independent and non-paired.
Procedure: Ethical approval was obtained from Faculty of Medicine at Umm Al-Qura University. The data were collected on April 2016 (one month before final exams) randomly from students who signed on consent forms. All statistical analysis done by SPSS ver. 23.
Results
The demographic and characteristics features of the students are shown in (Table 1).
In general, 71.4% had poor sleep quality (score greater than 5) ranged from 6-17 and 81.4% had depression (score greater than 4) ranged from 5-25. 19.5% report suicidal ideation at least once in last two weeks. The mean score for sleep quality was 7.47 ± 3.19 and the mean score for depression was 9.54 ± 5.32.
Highest level of poor sleep quality was in pharmacy students, with 75.3% followed by dentistry, 74.4% and lowest in medical students 68.76%. Highest level of depression was in dental students, 88.9% then medical students, 80.7% followed by pharmacy students 79%. Highest level of suicidal ideation was found in dentistry students, 35.6% followed by pharmacy and medicine 19.1% and 16.3% respectively (Table1).
About 31% of male had good sleep quality with mean score 7.14 ± 2.96 and (24.6%) had no depression with mean score 8.51 ± 5.1. Female were more likely to have depression and poor sleep quality than male. Highest level of depression among years was in second year and lowest in last year. Highest level of good sleep quality was in first year and lowest in fourth year. Single students had more depression 81.4% and better sleep quality 29%. There was more percentage of depression among students with low economic status (88.9%) and more percentage of poor sleep quality among students with medium economic status (75.7%). Students with health problem had more depression (86.8%) and worse sleep quality (77.9%). Students who smoke had more depression (86.7%) and worse sleep quality (74.7%) respectively. Student with very good GPA had better sleep quality (30.3%) and less depression (78.5%). Students who are regular in attending had less depression (79.7%) and better sleep quality (29.9%) respectively. Students who drink hot drinks daily had proportionally less depression (78.48%) and better sleep quality (31.2%) respectively. On other side students who drink cold drinks daily had more depression (83.87%) and worse sleep quality (80.6%) respectively. However no significant association were found between all these variables with sleep quality or depression except that gender was significantly associated with depression only. (Table 2).
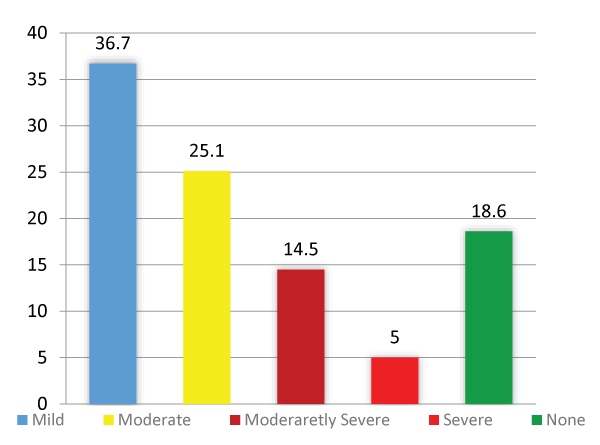
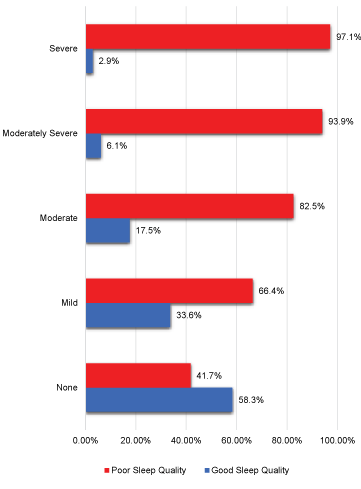
For severity of depression (36.7%) had mild depression, while (5%) had severe depression and (18.6%) had no depression (Figure 1). Increase severity of depression is significantly associated with sleep quality (p < 0.000) (Figure 2). Male students had less depression, better sleep quality than female, across, all three colleges except in dentistry. Highest level of severe depression was among medical students (Table 3).
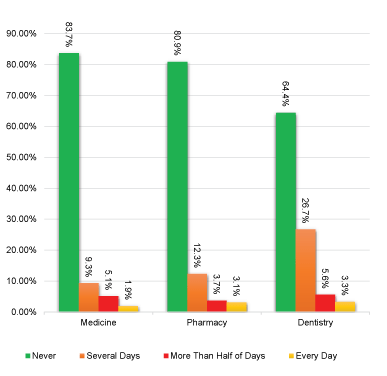
About 42% of students with no depression report poor sleep quality whereas 78.2% with depression had poor sleep quality. Students with depression, have 5 times risk to have poor sleep quality than who do not have depression. 85% of students with suicidal ideation report poor sleep quality whereas 68.1% of students who do not have suicidal ideation, had poor sleep quality. Suicidal ideation is 20 times risk to be associated with depression than who do not (OR 20:1). %). About 71% of students with severe depression (24 out of 34 students) had suicidal ideation. About 12.3% of students report suicidal ideation several days) and female report higher level of suicidal ideation than male (20.7% versus 18.3%), however there was no significant association between suicidal ideation with gender (p = 0.438). About 3% of dental students had suicidal ideation every day (Figure 3). Significant association was observed between depression, sleep quality and suicidal ideation with each other (p < 0.000) (Table 4).
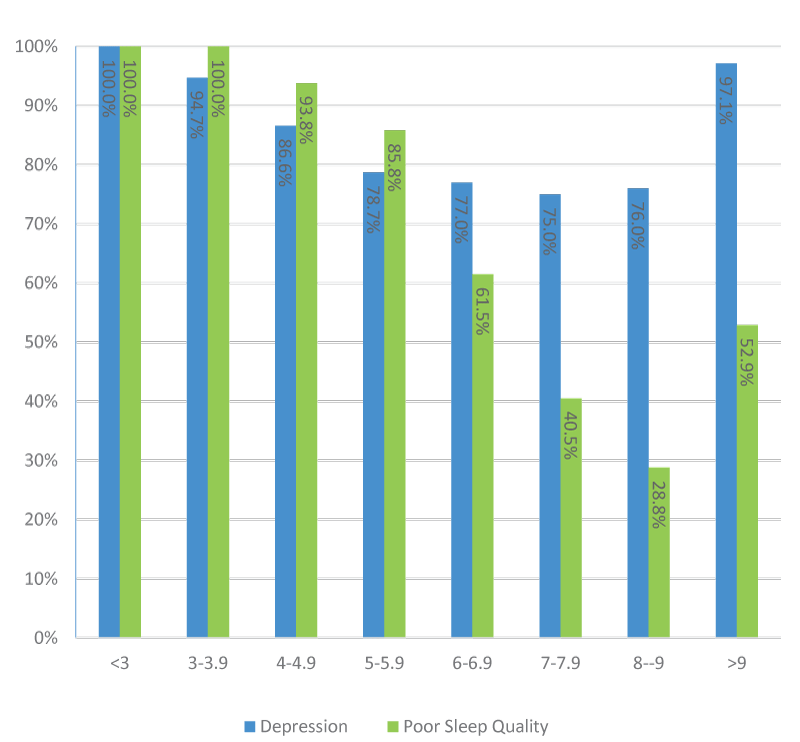
10.3% of student use sleep medication at least once in last month and male had higher rates than female (10.9% versus 9.6%) with no significant association between use of sleep medication with gender (p = 0.321). highest percentage was among dental students (12.2%). Only 5.7% of student who used sleep medication had good sleep quality and 90% of them had depression. Highest sleeping trouble reported by students were; cannot get to sleep within 30 minutes and wake up in middle of night or early morning by 69.8% and 64.2% respectively. About 63% of students’ sleep 4-6 hours, only and 6.2% sleep more than 8 hours. Most of students (47%) went to bed at 12:00AM-1:59 AM and most of students (36.1%) woke up at 7:00AM-7:59AM (Table 5). Mean sleeping hours is 5.65 (5 hours and 39 minutes) with male score 5.80 and female score 5.50. Lowest depression and best sleep quality was among student who sleep between 7 to 9 hours whereas depression and poor sleep quality increase in student who sleep less than 7 hours or even more than 9 hours (Figure 4). On Pearson correlation sleeping quality and depression were significantly and negatively correlated with sleeping duration (p = < 0.01).
For the seven PSQI components the worst scored by all students was sleep duration followed by sleep latency. Subjective sleep quality, sleep latency, sleep duration and habitual sleep efficiency were highest and worst among pharmacy students. Sleep disturbances and use of sleep medication were worst among dentistry and for daytime dysfunction was worst in dentistry. We used Kruskal-Wallis Test, only 2 components were significant that is sleep duration and daytime dysfunction, also the global PSQI score were significant according to colleges (Table 6). According to gender male was worse than female in only 2 components that is habitual sleep efficiency and use of sleep medication. We used Mann-Whitney Test sleep duration, sleep disturbances and daytime dysfunction were significant according to gender (Table 7).
Discussion
The aim of the present study was to find prevalence of sleep quality and depression among medical and allied medical sciences students and the relationship between sleep quality and depression.
In present study, a total of 681 students were assessed for their sleep quality, depression and suicidal ideation in three colleges of Umm Al-Qura University. Dentistry students performed poor in most of the risk indicators like cold drink daily use, depression and suicidal ideation as compare to medicine and pharmacy students. The male/female ratio of the studied population was 49.6:50.4 and most of them (60.2%) were from affluent families. Forty-six (6.8%) were married. Eighty-three (12.2%) were smokers.
Most of the students in the present study 71.4% had poor sleep quality, our result is close to Shad, 2015 who found it 72.9% and Afandi,2013 found it 67.2% [9,10]. Other similar Saudi studies conducted by Abdulghani et al, 2012 and Alsaggaf, 2016 recorded it as 36.6% and 30% respectively [8,11]. Serra-Negra,2014 found it 60.1% [12]. Kabrita,2014 found it 58.7% [13]. Lemma, 2012 found it 55.8% [14]. Cates, 2015 found it 55% [15]. Shu Hui, 2012 found it 54.7% [16]. Assaad, 2014 found it 53.2% [17]. Juan et al, 2013 found it 51.8% [18]. Lohsoonthorn, 2013 found it 48.1% [19]. Jain, 2013 found it 41.1% [20].
In present study, the mean score for global PSQI was 7.47 ± 3.19 while Kabrita, 2014 found it 6.57 ± 3.49 (13). Shad, 2015 who found it 6.45 ± 2.85 [9]. Shih Yu et al, 2013 found it 6.29 ± 2.98 [21]. Lemma,2012 found it 6.23 [14]. Cates, 2015 found it 6.19 ± 2.93 [15]. Serra-Negra, 2014 found it 6.08 ± 2.18 [12]. Shu Hui, 2012 recorded it as 6.0 ± 2.5 [16]. Our results are higher than what all other studies reported, probably the cause may be, the more complicated and difficult system in theses colleges, which ignore completely the psychological conditions of students, put them under pressure of studying, changing their habit, like studying all night, trying to study and cover all objectives of each subject, and also working on projects, which may result in poor sleep quality and depression that’s why we advise to establish a wellness unit in each college to help student how to deal with all these huge responsibilities.
In present study, female had more poor sleep quality than male which is similar to result found by Shad, 2015, Abdulghani et al, 2012, Juan et al, 2013 and Shu Hui, 2012 ([8,916], [18]. Other studies were opposite to our result that male had more poor sleep quality than female found by Cates, 2015, Afandi,2013 and Lohsoonthorn,2013 [10,15,19].
In present study mean sleep hours is 5 hours and 40 minutes (5.7 hours) which is close to 5.8 hours [11]. Kabrita,2014 found it 7.95 hours [13]. Shih Yu et al, 2013 found it 7 hours [21]. Cates, 2015 and Serra-Negra, 2014 found it 6.8 hours [12,15]. Lemma,2012 found it 6.79 hours [14]. Assaad,2014 found it 6.67 hours [17].
Similar to present study, previous studies found no significant association of sleep quality with gender, (9, 10, 13, 15, 17). academic year [15]. marital status [13]. economic status [13]. hot drinks [13,18]. smoking [10,16,18]. GPA [11]. and health problems [8,16]. In contrast to present study, previous studies found significant association of sleep quality with gender [8,16,18] academic year [9,12], hot drinks [16,19] cold drinks [10,18,19]. smoking [13] GPA [18,5] and regular attendance [10].
10.3% of students in present study use sleep medication which is close to 9% [11] while Serra-Negra, 2014 found it 5.5% [12]. and Lohsoonthorn,2013 found it 2% [19]. Assaad,2014 found it 21% and he support our finding that significant association of sleep quality with use of sleep medication and students who take sleep medication are at higher risk to be poor sleepers [17].
According to gender the present study found that out of the seven components of PSQI only 3 of it were significant which was sleep duration, sleep disturbances and daytime dysfunction and male worse than female in habitual sleep efficiency and use of sleep medication components. Cates, 2015 found that only sleep duration was significant and male worse than female in sleep duration, sleep latency and subjective sleep quality while Juan et al, 2013 found only sleep latency was significant [15,18].
In present study, we found the prevalence of depression as 81.4% among Umm Al-Qura University (UQU) students and the mean score for depression was 9.54 ± 5.32.
In previous studies conducted at UQU Khalid, 2015 and Jarwan,2015 found the prevalence of depression as 69.9% and 30.9% respectively [22,23]. While prevalence of depression in other studies conducted in Saudi Arabia universities were as follows; Inam, 2007 found it 50% in Qassim University students [24]. Al-Faris, 2012 found it 48.2% in King Saud University [25]. Kulsoom, 2015 found it 43% in Alfaisal University [26]. Ibrahim, 2013 found it 36.5% in King Abdul-Aziz University [27]. El-Gilany, 2008 found it 16.2% in King Faisal University [28]. In comparison to Non-Saudi. Bathla, 2015 found it 82.9% [29]. Khan, 2006 found it 70% [30]. Shi, 2016 found it 66.8% [31]. Sobowale, 2014 found it 64.9% with mean score 6.02 ± 3.44 PHQ-9 [32]. Ayat, 2014 found it 63.6% [33]. Singh, 2016 found it 59.8% [34]. Lemma,2012 found it 50.8% [14]. Dyrbye, 2008 found it 46.5% [35]. Jadoon,2010 found it 43.9% [36]. Baldassin, 2008 found it 38.2% [37]. Jeong, 2010 found it 37.1% [38]. Ahmed, 2009 found it 28.6% [39]. Bayram,2008 found it 27.1% [40]. Mellal, 2014 found it 22.2% [41]. Al Busaidi, 2011 found it 17% [42]. Dahlin, 2005 found it 12.9% [43]. Galen, 2014 found it 9.5% [44]. Coentre, 2016 found it 7.9% [45].
Similar to present study previous studies found no significant association of depression with academic year [27, 32,41, 42], marital status [25.36,41], economic status [29,36,38], smoking [38,41]and GPA [25,41]. In contrast to present study, previous studies found significant association of depression with academic year [24,25,30,36,37], marital [27], economic status [25,27,29,33,41], smoking [26], health problems and hot drinks [43].
In present study, we found significant association of depression with gender which is supported by many study [25,30,31,33,36,37,40] while other studies not support this association [23,24,26,44]. Many studies found male had more depression than female [30,31,33]. Unlike present study and other similar studies [23-26,36,37,41,43,45].
In present study 19.5% of students had suicidal ideation. Dahlin, 2005 found it 28.8% and 2.7% attempt to suicide [43]. Clark, 1988 found it between 15-20% [46]. Tyssen, 2001 found it 14.5% and 1.4% attempt to suicide [47]. Dyrbye, 2008 found it 11.2% and 1.9% attempt to suicide [35]. Galen, 2014 found it 8.5% [44]. Sobowale, 2014 found it 7.5% [32]. Coentre, 2016 found it 3.7% and 0.7% attempt to suicide [45].
In present study, both sleep quality and depression are associated with increased risk of suicide which is similar to previous studies [32,35,44, 45] and poor sleep quality [48].
Limitations of the study: We wanted to include all departments of Allied medical sciences but could not get permission from the applied medical sciences, hence the result represent the high depression rate in medical, pharmacy and dental students.
Conclusion
We found a very high prevalence of poor sleep quality and depression in Umm Al-Qura University medical and allied students. Similarly the percentage of suicidal ideation was also high. It may be due to shift application of teaching methodology and content from traditional to reformed curriculum. Further students should be conducted to find out the perception of students and teaching faculty regarding the risk and protective factors for high prevalence of depression, poor sleep quality and suicidal ideation.
- Buxton OM, Marcelli E. Short and long sleep are positively associated with obesity, diabetes, hypertension, and cardiovascular disease among adults in the United States. Soc Sci Med. 2010; 71: 1027-1036. DOI: 10.1016/j.socscimed.2010.05.041
- Buysse DJ. Sleep health: can we define it? Does it matter? Sleep. 2014; 37: 9-17. DOI: 10.5665/sleep.3298
- Gottlieb DJ, O'Connor GT, Wilk JB. Genome-wide association of sleep and circadian phenotypes. BMC Med Genet. 2007; 8: 9. https://bit.ly/39b3nxr
- Williamson AM, Feyer AM. Moderate sleep deprivation produces impairments in cognitive and motor performance equivalent to legally prescribed levels of alcohol intoxication. Occup Environ Med. 2000; 57: 649-655. DOI: 10.1136/oem.57.10.649
- Krystal AD. Psychiatric disorders and sleep. Neurol Clin. 2012; 30:1389-1413.DOI: 10.1016/j.ncl.2012.08.018
- Buysse DJ, Reynolds CF, 3rd, Monk TH, Berman SR, Kupfer DJ. The Pittsburgh Sleep Quality Index: A new instrument for psychiatric practice and research. Psychiatry Res. 1989; 28: 193-213. DOI: 10.1016/0165-1781(89)90047-4
- K K, RL S. The PHQ-9: A new depression diagnostic and severity measure. Psychiatric Annals. 2002; 32: 6. https://bit.ly/32N596P
- Shad R, Thawani R, Goel A. Burnout and sleep quality: A cross-sectional questionnaire-based study of medical and non-medical students in India. Cureus. 2015; 7: 361. DOI: 10.7759/cureus.361
- Afandi O, Hawi H, Mohammed L, Salim F, Hameed AK, Shaikh RB, et al. Sleep quality among university students: evaluating the impact of smoking, social media use, and energy drink consumption on sleep quality and anxiety. Inquiries. 2013; 5. https://bit.ly/3hibDOK
- Abdulghani HM, Alrowais NA, Bin-Saad NS, Al-Subaie NM, Haji AM, Alhaqwi AI. Sleep disorder among medical students: Relationship to their academic performance. Med Teach. 2012; 34: 37-41. DOI: 10.3109/0142159X.2012.656749
- Alsaggaf MA, Wali SO, Merdad RA, Merdad LA. Sleep quantity, quality, and insomnia symptoms of medical students during clinical years. Relationship with stress and academic performance. Saudi Med J. 2016; 37: 173-182. DOI: 10.15537/smj.2016.2.14288
- Serra-Negra JM, Scarpelli AC, Tirsa-Costa D, Guimaraes FH, Pordeus IA, Paiva SM. Sleep bruxism, awake bruxism and sleep quality among Brazilian dental students: a cross-sectional study. Braz Dent J. 2014; 25: 241-247. https://bit.ly/3eKNZcj
- Kabrita CS, Hajjar-Muca TA, Duffy JF. Predictors of poor sleep quality among Lebanese university students: Association between evening typology, lifestyle behaviors, and sleep habits. Nat Sci Sleep. 2014; 6: 11-18. DOI: 10.2147/NSS.S55538
- Lemma S, Gelaye B, Berhane Y, Worku A, Williams MA. Sleep quality and its psychological correlates among university students in Ethiopia: A cross-sectional study. BMC Psychiatry. 2012; 12: 237. https://bit.ly/32yQhZl
- Cates ME, Clark A, Woolley TW, Saunders A. Sleep quality among pharmacy students. Am J Pharm Educ. 2015; 79: 9. DOI: 10.5688/ajpe79109
- Cheng SH, Shih CC, Lee IH, Hou YW, Chen KC, Chen KT, et al. A study on the sleep quality of incoming university students. Psychiatry Res. 2012; 197: 270-274. DOI: 10.1016/j.psychres.2011.08.011
- Assaad S, Costanian C, Haddad G, Tannous F. Sleep patterns and disorders among university students in Lebanon. J Res Health Sci. 2014; 14: 198-204. https://bit.ly/30rjQJU
- Velez JC, Souza A, Traslavina S, Barbosa C, Wosu A, Andrade A, et al. The epidemiology of sleep quality and consumption of stimulant beverages among patagonian chilean college students. Sleep Disord. 2013; 2013: 910104. DOI: 10.1155/2013/910104
- Sanchez SE, Martinez C, Oriol RA, Yanez D, Castaneda B, Sanchez E, et al. Sleep Quality, Sleep Patterns and Consumption of Energy Drinks and Other Caffeinated Beverages among Peruvian College Students. Health (Irvine Calif). 2013; 5: 26-35. DOI: 10.4236/health.2013.58A2005
- Jain V, Tomar R, Jha J, Pareek A, Ratan Y, Paliwal N. Sleep quality and sleep associated problems in female pharmacy students. Chronicles of Young Scientists. 2013; 4: 138-143. https://bit.ly/32NbizV
- Lee SY, Wuertz C, Rogers R, Chen YP. Stress and sleep disturbances in female college students. Am J Health Behav. 2013; 37: 851-858. DOI: 10.5993/AJHB.37.6.14
- Aboalshamat K, Hou X-Y, Strodl E. Psychological well-being status among medical and dental students in Makkah, Saudi Arabia: A cross-sectional study. Medical Teacher. 2015; 37: 75-81. DOI: 10.3109/0142159X.2015.1006612
- BK J. Depression among medical students of Faculty of Medicine, Umm Al-Qura University in Makkah, Saudi Arabia. International Journal of Medical Science and Public Health. 2015; 4. https://bit.ly/39cTejz
- Inam SB. Anxiety and Depression among Students of a Medical College in Saudi Arabia. Int J Health Sci (Qassim). 2007; 1: 295-300. https://bit.ly/3jhmfiZ
- Al-Faris EA, Irfan F, Van der Vleuten CP, Naeem N, Alsalem A, Alamiri N, et al. The prevalence and correlates of depressive symptoms from an Arabian setting: A wake up call. Med Teach. 2012; 34: 32-36. DOI: 10.3109/0142159X.2012.656755.
- Kulsoom B, Afsar NA. Stress, anxiety, and depression among medical students in a multiethnic setting. Neuropsychiatr Dis Treat. 2015; 11: 1713-1722. DOI: 10.2147/NDT.S83577
- Ibrahim N, Al-Kharboush D, El-Khatib L, Al-Habib A, Asali D. Prevalence and Predictors of Anxiety and depression among female medical students in King Abdulaziz University, Jeddah, Saudi Arabia. Iran J Public Health. 2013; 42: 726-736. https://bit.ly/3fNEnP2
- El-Gilany AH, Amr M, Hammad S. Perceived stress among male medical students in Egypt and Saudi Arabia: effect of sociodemographic factors. Ann Saudi Med. 2008; 28: 442-448. DOI: 10.5144/0256-4947.2008.442
- Bathla M, Singh M, Kulhara P, Chandna S, Aneja J. Evaluation of anxiety, depression and suicidal intent in undergraduate dental students: A cross-sectional study. Contemp Clin Dent. 2015; 6: 215-222. DOI: 10.4103/0976-237X.156050
- Khan MS, Mahmood S, Badshah A, Ali SU, Jamal Y. Prevalence of depression, anxiety and their associated factors among medical students in Karachi, Pakistan. J Pak Med Assoc. 2006; 56: 583-586. https://bit.ly/30rAOI7
- Shi M, Liu L, Wang ZY, Wang L. Prevalence of depressive symptoms and its correlations with positive psychological variables among Chinese medical students: an exploratory cross-sectional study. BMC Psychiatry. 2016; 16: 3. DOI: 10.1186/s12888-016-0710-3
- Sobowale K, Zhou N, Fan J, Liu N, Sherer R. Depression and suicidal ideation in medical students in China: A call for wellness curricula. Int J Med Educ. 2014; 5: 31-36. DOI: 10.5116/ijme.52e3.a465
- Abdallah AR, Gabr HM. Depression, anxiety and stress among first year medical students in an Egyptian public university. International Research Journal of Medicine and Medical Sciences. 2014; 2: 11-19. https://bit.ly/2WBqBaR
- Singh Manpreet BM, Chandna S, Singh Surjeet, Cholera Rashmin. Evaluation of Anxiety, Depression and Suicidal Intent in Medical Undergraduate Students in Northern India: A Cross Sectional Study. Sch. J. App. Med. Sci. 2016; 4: 712-720. DOI: 10.4103/0976-237X.156050
- Dyrbye LN, Thomas MR, Massie F. BUrnout and suicidal ideation among u.s. medical students. Annals of Internal Medicine. 2008; 149: 334-341. DOI: 10.7326/0003-4819-149-5-200809020-00008
- Jadoon NA, Yaqoob R, Raza A, Shehzad MA, Zeshan SC. Anxiety and depression among medical students: A cross-sectional study. JPMA The Journal of the Pakistan Medical Association. 2010; 60: 699-702. https://bit.ly/2ZKAwNq
- Baldassin S, Alves TC, de Andrade AG, Nogueira Martins LA. The characteristics of depressive symptoms in medical students during medical education and training: a cross-sectional study. BMC Med Educ. 2008; 8: 60. DOI: 10.1186/1472-6920-8-60
- Jeong Y, Kim JY, Ryu JS, Lee KE, Ha EH, Park H. The associations between social support, health-related behaviors, socioeconomic status and depression in medical students. Epidemiol Health. 2010; 32: 2010009. DOI: 10.4178/epih/e2010009
- Ahmed I, Banu H, Al-Fageer R, Al-Suwaidi R. Cognitive emotions: Depression and anxiety in medical students and staff. J Crit Care. 2009; 24: 1-7. DOI: 10.1016/j.jcrc.2009.06.003
- Bayram N, Bilgel N. The prevalence and socio-demographic correlations of depression, anxiety and stress among a group of university students. Soc Psychiatry Psychiatr Epidemiol. 2008; 43: 667-672. DOI: 10.1007/s00127-008-0345-x
- Mellal AA, Albluwe T, Al-Ashkar D. The prevalence of depressive symptoms and its socioeconomic determinants among university students in al ain, UAE. International Journal of Pharmacy and Pharmaceutical Sciences. 2014; 6. https://bit.ly/32C03du
- Al-Busaidi Z, Bhargava K, Al-Ismaily A, Al-Lawati H, Al-Kindi R, Al-Shafaee M, et al. Prevalence of depressive symptoms among university students in oman. Oman Med J. 2011; 26: 235-239. DOI: 10.5001/omj.2011.58
- Dahlin M, Joneborg N, Runeson B. Stress and depression among medical students: A cross-sectional study. Med Educ. 2005; 39: 594-604. DOI: 10.1111/j.1365-2929.2005.02176.x
- Galan F, Rios-Santos JV, Polo J, Rios-Carrasco B, Bullón P. Burnout, depression and suicidal ideation in dental students. Medicina Oral, Patologia Oral y Cirugia Bucal. 2014; 19: 206-211. DOI: 10.4317/medoral.19281
- Coentre R, Faravelli C, Figueira ML. Assessment of depression and suicidal behaviour among medical students in Portugal. International Journal of Medical Education. 2016; 7: 354-363. DOI: 10.5116/ijme.57f8.c468
- Clark DC, Zeldow PB. Vicissitudes of depressed mood during four years of medical school. JAMA. 1988; 260: 2521-2528. https://bit.ly/39abmuA
- Tyssen R, Vaglum P, Gronvold NT, Ekeberg O. Suicidal ideation among medical students and young physicians: A nationwide and prospective study of prevalence and predictors. J Affect Disord. 2001; 64: 69-79. DOI: 10.1016/s0165-0327(00)00205-6
- Bernert RA, Turvey CL, Conwell Y, Joiner TE, Jr. Association of poor subjective sleep quality with risk for death by suicide during a 10-year period: A longitudinal, population-based study of late life. JAMA Psychiatry. 2014; 71: 1129-1137. DOI: 10.1001/jamapsychiatry.2014.1126

Sign up for Article Alerts